..
Excerpts from:
MAY 26, 2020
First results from human COVID-19 immunology study reveal universally effective antibodies
The first round of results from an immunological study of 149 people who have recovered from COVID-19 show that although the amount of antibodies they generated varies widely, most individuals had generated at least some that were intrinsically capable of neutralizing the SARS-CoV-2 virus.
Antibodies vary widely in their efficacy. While many may latch on to the virus, only some are truly “neutralizing,” meaning that they actually block the virus from entering the cells.
Since April 1, a team of immunologists, medical scientists, and virologists, has been collecting blood samples from volunteers who have recovered from COVID-19. The majority of the samples they have studied showed poor to modest “neutralizing activity,” indicating a weak antibody response. However, a closer look revealed everyone’s immune system is capable of generating effective antibodies—just not necessarily enough of them. Even when neutralizing antibodies were not present in an individual’s serum in large quantities, researchers could find some rare immune cells that make them.
“This suggests just about everybody can do this, which is very good news for vaccines,” says Michel C. Nussenzweig, head of the Laboratory of Molecular Immunology at Rockefeller. “It means if you were able to create a vaccine that elicits these particular antibodies, then the vaccine is likely to be effective and work for a lot of people.”
Moreover, the researchers identified three distinct antibodies that were shown to be the most potent of the bunch in neutralizing the virus. They are working to develop them further into therapeutic and preventive drugs.
The findings are shared on BioRxiv ahead of submission to peer-reviewed scientific journals. Nussenzweig’s collaborators include, Davide F. Robbiani, Marina Caskey, Paul Bieniasz, Theodora Hatziioannou, and Charles M. Rice.
https://medicalxpress.com/news/2020-05-results-human-covid-immunology-reveal.html
..
Excerpts from:
The study was carried out on 160 members of staff at two hospital sites in Strasbourg who had all tested positive for COVID-19 and suffered mild forms of the disease.
MAY 26, 2020
Even mild coronavirus illness may confer some immunity: study
Even people with minor illness from the coronavirus can develop antibodies that could leave them immunised for several weeks or more, according to an early French study that tested hospital staff with mild infections.
Researchers said the results, which have not yet been peer reviewed, were “encouraging” since little is known about the mechanisms of immunity against the novel coronavirus, especially in people with minor forms of the disease.
“We knew that people with severe forms of the disease developed antibodies within 15 days of the onset of symptoms,” said Arnaud Fontanet, head of the global health department at the Institut Pasteur, which conducted the research with the University Hospital in Strasbourg.
“We now know that this is also true for those who develop minor forms, even if the rates of antibodies are probably weaker.”
The study was carried out on 160 members of staff at two hospital sites in Strasbourg who had all tested positive for COVID-19 and suffered mild forms of the disease.
Two types of serological tests, which aim to look for a previous infection, indicated that almost all health workers—153 out of 160 in one case, 159 out of 160 in the other—had developed antibodies within 15 days after the onset of infection.
Using a separate test to determine if the antibody could neutralise the virus, the study found some 98 percent of the volunteers had these antibodies between 28 and 41 days after the first signs of infection.
The researchers said in a statement on Tuesday that the neutralising activity of the antibodies appeared to increase over time.
https://medicalxpress.com/news/2020-05-mild-coronavirus-illness-confer-immunity.html
..
Coronavirus patients declared recovered who later test positive for the disease are still expelling dead lung cells rather than getting a new infection, the World Health Organization (WHO) told AFP on Wednesday.
South Korean health officials reported more than 100 such cases in April, raising concerns that patients who had recovered could become reinfected.
“We are aware that some patients test positive after they clinically recover,” a WHO spokesperson told AFP, without making specific reference to the South Korean cases.
“From what we currently know—and this is based on very recent data—it seems they these patients are expelling left over materials from their lungs, as part of the recovery phase.”
People infected with the new coronavirus build up antibodies starting a week or so after infection or the onset of symptoms, research has shown.
But it is still not clear, experts say, whether the body systematically builds up enough immunity to ward off a new attack by the virus or, if it does, how long such immunity lasts.
As for the recovered patients who tested negative and then, weeks later, positive, more research is needed, according to the WHO.
https://medicalxpress.com/news/2020-05-positive-recovered-virus-patients-reinfections.html
..
NEW YORK (NYTIMES) – A new study offers a glimmer of hope in the grim fight against the coronavirus: Nearly everyone who has had the disease – regardless of age, sex or severity of illness – makes antibodies to the virus.
The study, posted online on Tuesday (May 5) but not yet reviewed by experts, also hints that anyone who has recovered from infection may safely return to work – although it is unclear how long their protection might last.
“This is very good news,” said Angela Rasmussen, a virologist at Columbia University in New York who was not involved with the work.
..
Excerpts from:
Even as virologists zero in on the virus that causes COVID-19, a very basic question remains unanswered: do those who recover from the disease have immunity?
There is no clear answer to this question, experts say, even if many have assumed that contracting the potentially deadly disease confers immunity, at least for a while.
“Being immunised means that you have developed an immune response against a virus such that you can repulse it,” explained Eric Vivier, a professor of immunology in the public hospital system in Marseilles.
“Our immune systems remember, which normally prevents you from being infected by the same virus later on.”
For some viral diseases such a measles, overcoming the sickness confers immunity for life.
But for RNA-based viruses such as Sars-Cov-2—the scientific name for the bug that causes the COVID-19 disease—it takes about three weeks to build up a sufficient quantity of antibodies, and even then they may provide protection for only a few months, Vivier told AFP.
At least that is the theory. In reality, the new coronavirus has thrown up one surprise after another, to the point where virologists and epidemiologists are sure of very little.
“We do not have the answers to that—it’s an unknown,” Michael Ryan, executive director of the World Health Organization’s Emergencies Programme said in a press conference this week when asked how long a recovered COVID-19 patient would have immunity.
“We would expect that to be a reasonable period of protection, but it is very difficult to say with a new virus—we can only extrapolate from other coronaviruses, and even that data is quite limited.”
–
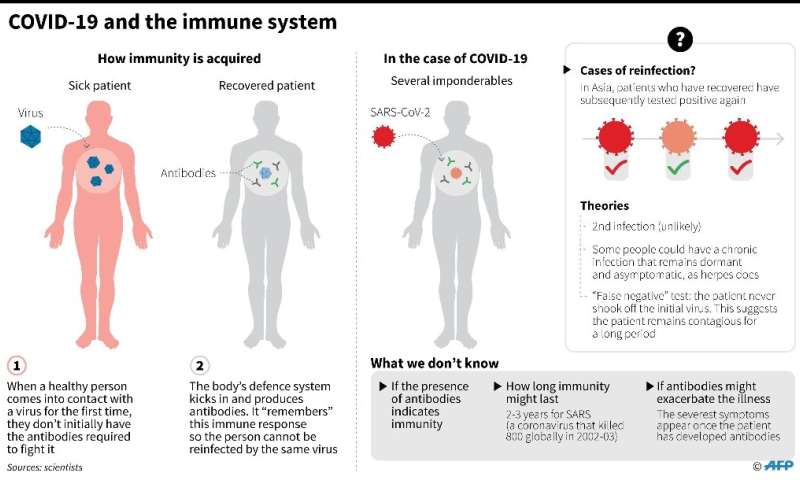
https://medicalxpress.com/news/2020-04-recovery-coronavirus-confer-immunity-experts.html
..
Antibodies are generated by the immune system and have unique chemical structures to inhibit specific pathogens. The coronavirus antibody intercepts the spike protein on the viral envelope to prevent it from binding with human cells.
https://www.scmp.com/news/china/science/article/3078840/coronavirus-low-antibody-levels-raise-questions-about
Excerpts from:
A team from Fudan University analysed blood samples from 175 patients discharged from the Shanghai Public Health Clinical Centre and found that nearly a third had unexpectedly low levels of antibodies.
In some cases, antibodies could not be detected at all.
“Whether these patients were at high risk of rebound or reinfection should be explored in further studies,” the team wrote in preliminary research released on Monday on Medrxiv.org, an online platform for preprint papers.
Although the study was preliminary and not peer-reviewed, it was the world’s first systematic examination of antibody levels in patients who had recovered from Covid-19, the disease caused by the coronavirus, the researchers said.
..
Fifty-one patients who recovered from coronavirus in South Korea have tested positive again, raising fears the virus can be reactivated.
The patients – from the country’s worst-hit city, Daegu – were put in quarantine after being diagnosed with the virus, then tested positive again days being released.
Korea’s Centers for Disease Control and Prevention (KCDC) said the virus was likely ‘reactivated’, rather than patients becoming re-infected.
Scientists at the Government-run health body believe the virus may lay dormant at undetectable levels in human cells.
They say that for unknown reasons the viral particles can then be reactivated – but it is unclear if patients become infectious again.
Experts say there is no evidence to prove that the virus acts in this way and studies in monkeys have actually shown the opposite.
And they say in cases where patients produce a positive result twice, it is normally because of a test giving the wrong result, which happens one in five times.
https://www.dailymail.co.uk/news/article-8192015/Fifty-one-recovered-coronavirus-patients-test-positive-South-Korea.html?ito=social-twitter_mailonline
..
Peter Kolchinsky, virologist, writes on Covid-19 “reinfections” in Asia…
Posted on March 30, 2020
If you are hearing about #covid19 “reinfections” in Asia, I can offer you my take as a virologist. The best explanation for what we’re seeing is likely due to three things…
1) The patients have likely indeed recovered from their covid infection and are on their way to clearing the virus as their immune system hunts down every infected cell and stray virion. But there are still lingering bits and pieces of the virus around.
2) these tests can be very sensitive at detecting viral genetic material, even it’s just a non-infectious byproduct of the immune system conquering the virus.
3) but it’s also sometimes the case that the test yields a false negative result; maybe the swab didn’t pick up enough material or was mishandled, so the next retest turning up positive could be catching the original infection, not a new one.
Any responsible coverage of these “reinfection” rumors makes the point that we should not assume that these recovered patients actually were reinfected again or even that the low levels of viral material detected means they are infectious to others.
For example, NPR writes “It is unclear whether they are infectious and why they tested positive after their earlier negative test.”
..
